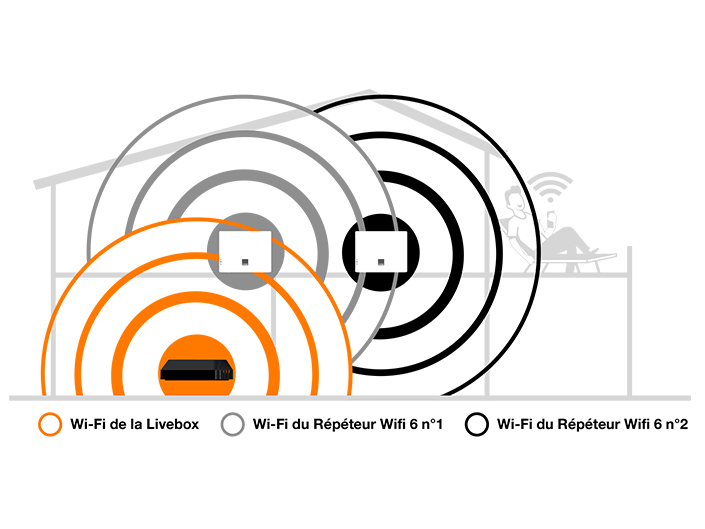
Augmentez la zone de couverture de votre réseau wifi et booster votre connexion. 🚀🚀🚀 Prix:13000f Téléphone : 774401042 #wifi #orange… | Instagram

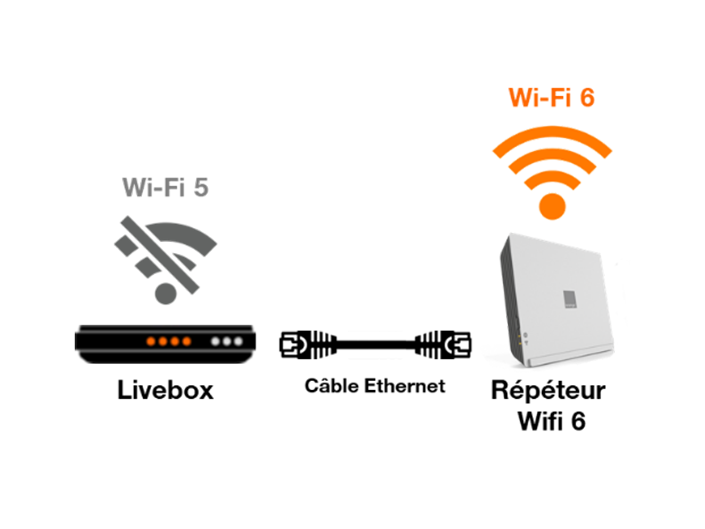
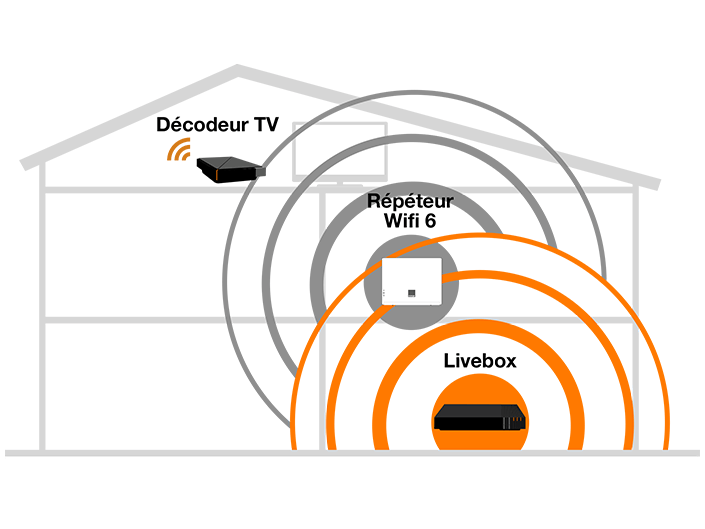
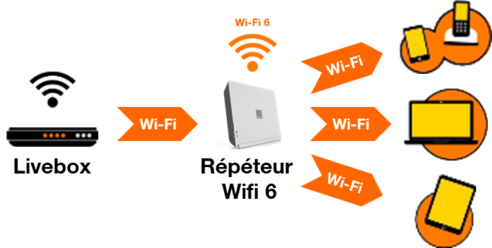
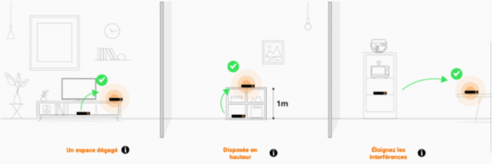
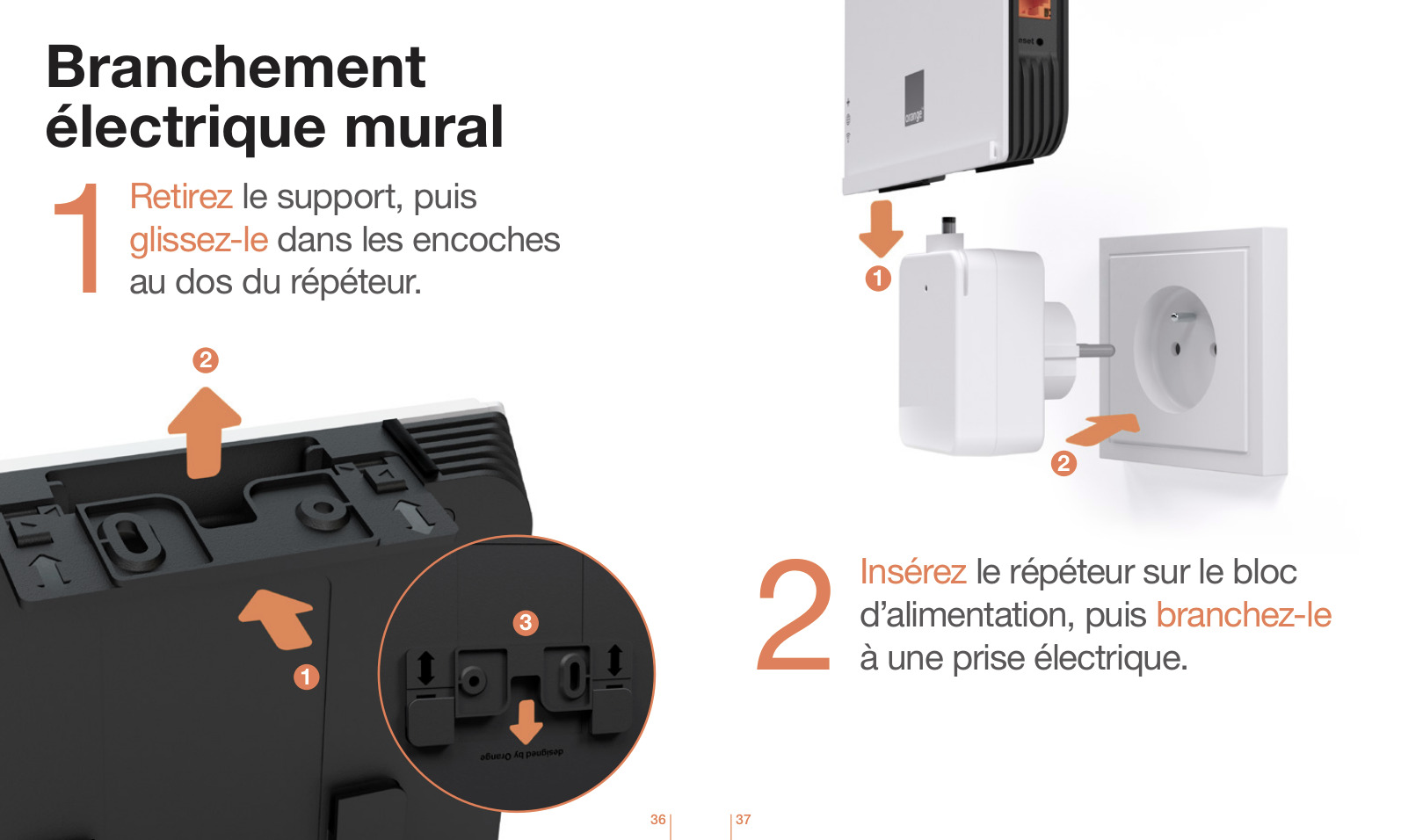
Orange - Étendez la zone de couverture wifi de votre Livebox et profitez d' Internet partout où vous en avez besoin ! Discret, ce répéteur wifi trouvera sa place n'importe où dans votre