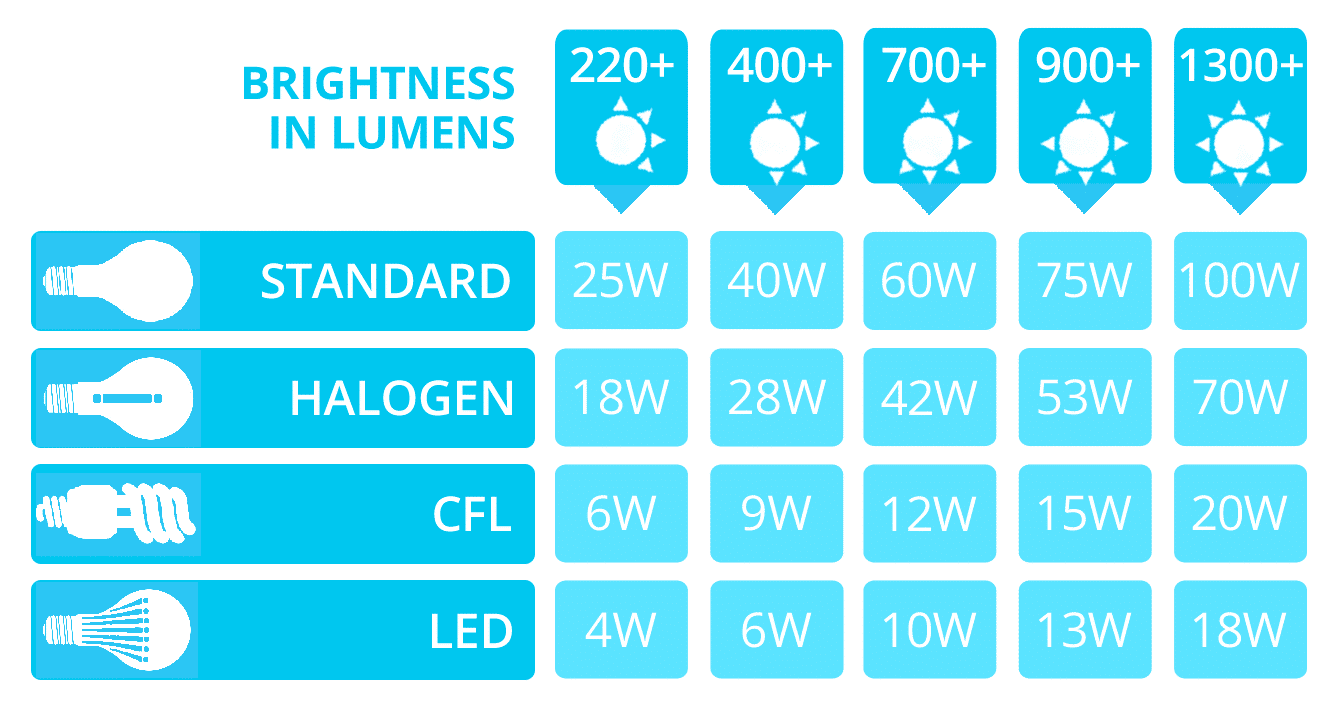
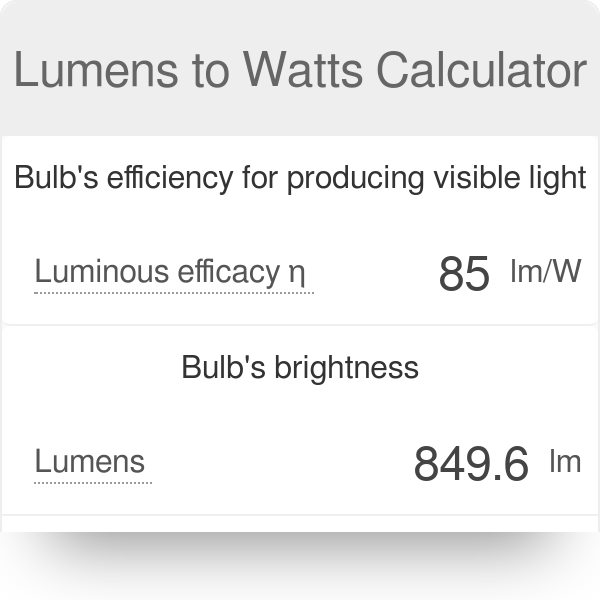
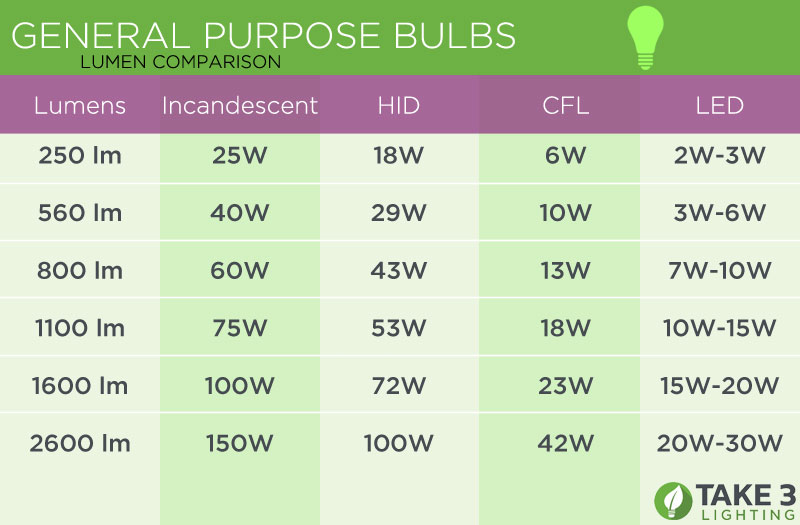
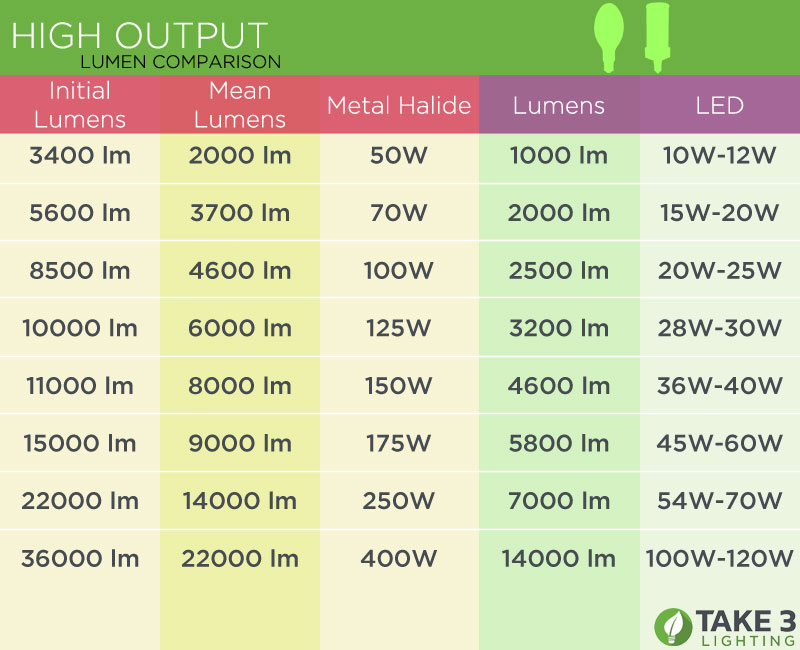
LED Flood Light Black 20-Watt 120v-277v 1850 Lumens 5000K 110 Degree Beam Spread | FL01-20W-50-BK | Destination Lighting

GE Lighting 38446 LED Flood/Security Bulb, Par30, Soft White, Long Neck, 1000 Lumens, 12-Watt - Quantity 1 - Amazon.com

A21 LED Light Bulbs, 23 Watts, 50-100-150 Equivalent Daylight White 5000K 600lm-1250lm-1850lm E26 Medium Base for Home Lighting Commercial Lighting 2 Pack - Walmart.com

6 Bulbs) GE 39277 LED 4-Pin CFL Replacement, 3000K Warm White, 18.5 watt, 1850 lumens LED Lightbulb - Amazon.com

GoodBulb 26 Watt Replacement Vertical LED Plug-in Light Bulbs | Commercial 16 Watt Type A 4 Pin G24Q Base 4000K Cool White | High Output 1850 Lumens | 140° Beam LED PL Light Bulbs | 10 Pack - Amazon.com

Satco S11828 24WLED/DW/EL/8/CCT-SEL/RND/RD - 8 Inch Ultra Slim Canless LED Recessed Light, Round, 24 Watt, 1850 Lumens, Selectable CCT, 2700K to 5000K, Remote Driver - Bees Lighting

Craftmade 1850-Lumen 25-Watt White Hardwired LED Flood Light in the Spot & Flood Lights department at Lowes.com

3-Way Soft White Light Bulb, 550/1300/1850 Lumens, 50/100/150-Watts - In Steubenville, OH - M&M True Value Hardware