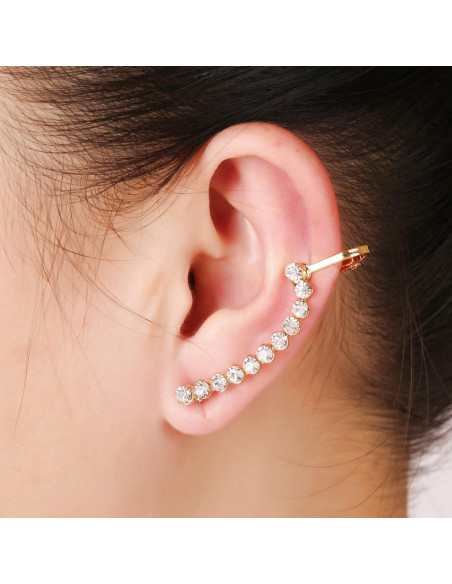
1 buc cruce manșetă de ureche cercei tassel pietre piercing-ul stud cercel simplu lanț clip cercei cuff 2022 femei trendy bijuterii cumpara online | Moda Bijuterii - Rebelstore.ro

Femei de Moda Linie Pietre Zircon Cercei Ureche Stud Clip Bijuterii Cercel pentru Ureche Clip Cercei Stud Cercei cerc reducere ~ Cercei > www.morcoveata.ro

La reducere! 80% fierbinte de vânzare de moda pentru femei cercei linie pietre zircon cercei ureche stud clip bijuterii aur feliuta серьги женские \ Cercei - www.babygreen.ro

Cercel pentru toata urechea, tip ear cuff, model cu frunze, pietre zirconiu, pentru partea stanga, placat cu aur 18K, argintiu - eMAG.ro

1 buc cruce manșetă de ureche cercei tassel pietre piercing-ul stud cercel simplu lanț clip cercei cuff 2022 femei trendy bijuterii cumpara online | Moda Bijuterii - Rebelstore.ro