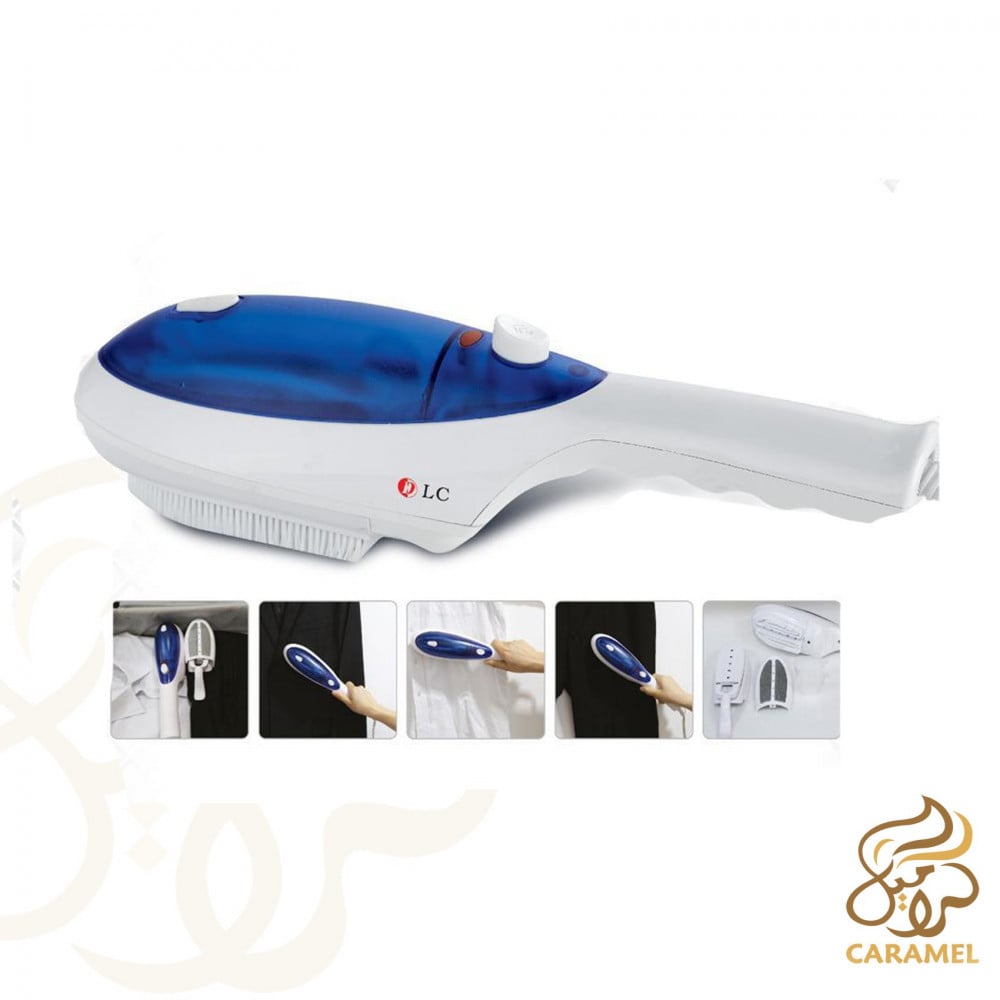
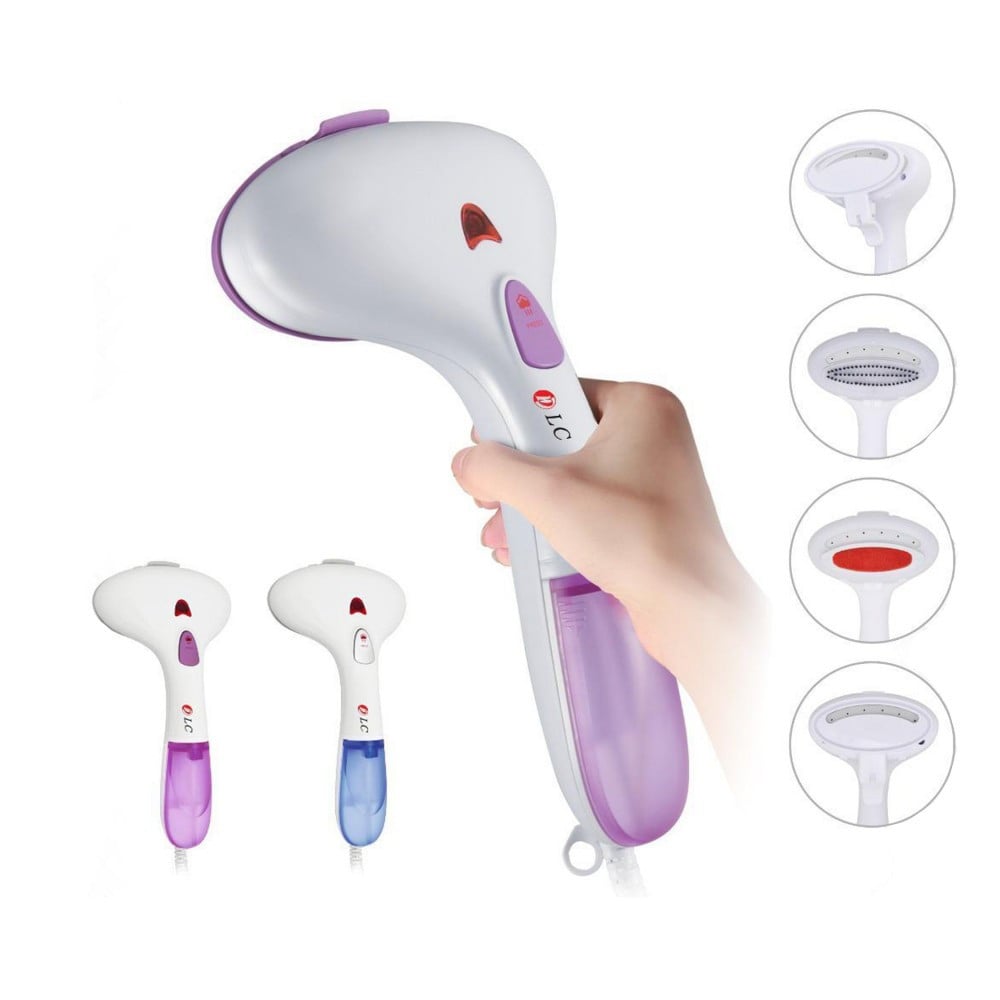
اشتري اونلاين بأفضل الاسعار بالسعودية - سوق الان امازون السعودية: مكواة بخار دي ال سي 1500 وات متعدد الالوان : المنزل والمطبخ

مكواة بخار للملابس المنزلية ، مصنوعة من قماش ناعم الملمس ، لكي الملابس|laundry ironing|touche clothinglaundry fabric - AliExpress

مكواة بخار من ارابيست، 1500 واط 350 مل، مكواة بخار منزلية محمولة صغيرة، للكي العمودي، تسخين سريع، فصل تلقائي للطاقة، لكي الملابس الكي بالبخار في المنزل والمكتب والسفر: اشتري اون لاين بأفضل

سعر مكواة بخار من شركة امجوي ، لون ابيض - موديل UEGS-407 فى السعودية | بواسطة امازون السعودية | كان بكام

سعر مكواة بخار الملابس من كليكون - 1700 واط - CK4033 فى السعودية | بواسطة امازون السعودية | كان بكام