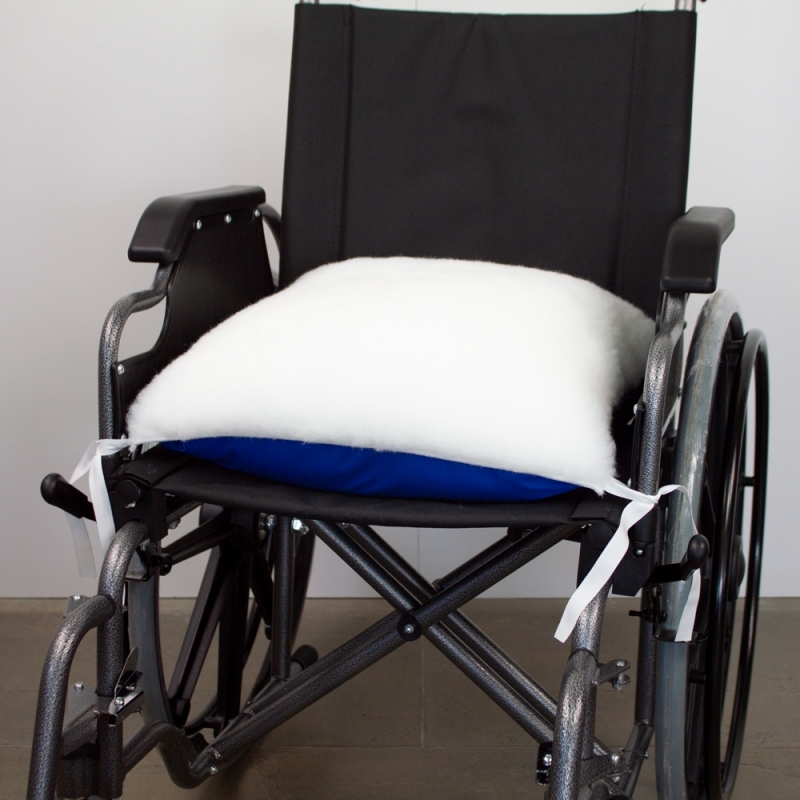
Acheter Coussin de siège anti-escarres pour fauteuil roulant - Trulife | Livraison gratuite, livré demain. - Soins à Domicile Webshop

Coussin anti-escarre forme fer à cheval Tech goural OSL1110 : Distributeur national EXCLUSIF d'orthèses auprès des particuliers et professionnels

Coussin anti-escarres pour fauteuil roulant Ymiko Coussin anti-escarres pour patient alité | Walmart Canada

Fauteuil roulant à pousser avec accessoires et assise anti escarres à découvrir et à essayer dans notre magasin de Toulon quartier Saint Jean du Var - ▷ Matériel médical | Location

Coussin de chaise,Coussin de Gel Respirant, Coussin Anti Escarres, Soulage la Pression sur Le Orthopédique avec Housse Antidérapant pour Voiture/Bureau/Maison/Fauteuil Roulant (noir) | Walmart Canada

Coussin anti-escarres pour fauteuil roulant avec mousse viscoélastique à mémoire de forme - Soins à Domicile Webshop