Amazon.com: Coros PACE 2 - Reloj deportivo GPS de alta calidad con correa de nailon o silicona, monitor de frecuencia cardíaca, batería GPS completa de 30 horas, barómetro, conexiones ANT+ y BLE,

En STOCK Ticwatch E2 reloj inteligente GPS reloj Strava Wear OS por Google 5ATM impermeable 24 horas Monitor de ritmo cardíaco Smartwatch hombres - AliExpress Productos electrónicos

Cómo Sincronizar Un Reloj Huawei Con Strava: Configuración Y Precio Para Unificar Tus Datos De Salud | sptc.edu.bd

2 # Relojes INTELIGENTES Deportivos con STRAVA. BICI 🚵♂️/\ NOTA 9 . Mejor Que GARMIN o POLAR - YouTube

Cómo sincronizar un reloj Huawei con Strava: configuración y precio para unificar tus datos de salud

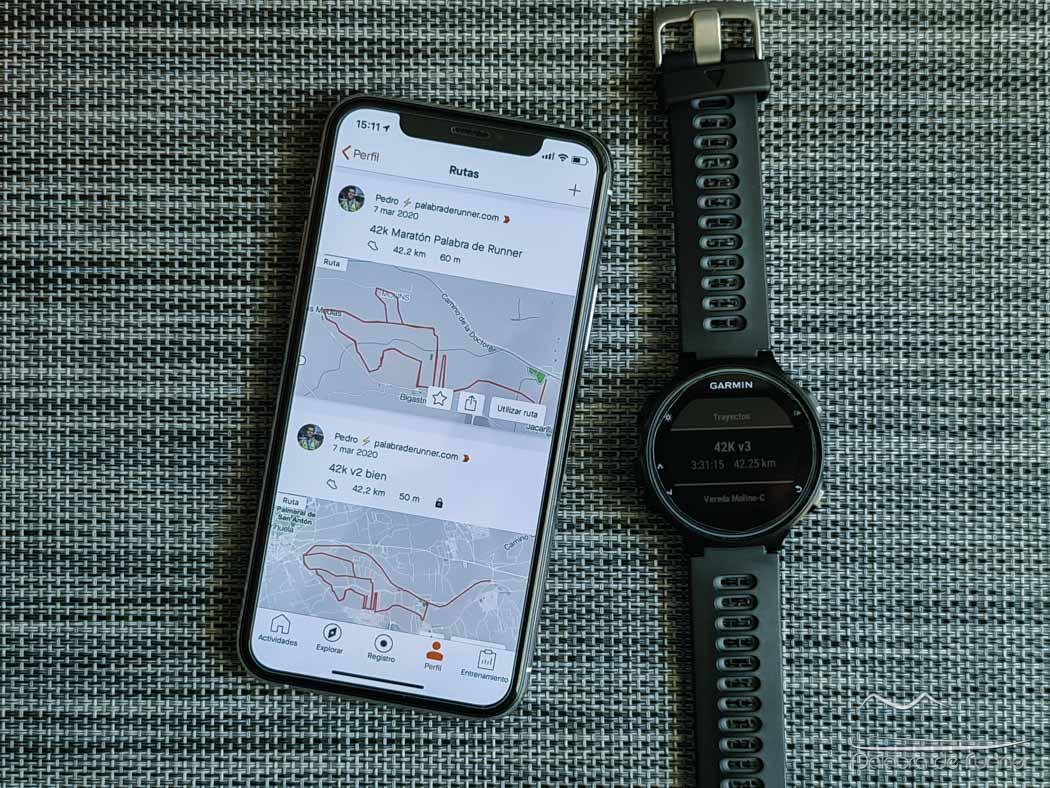
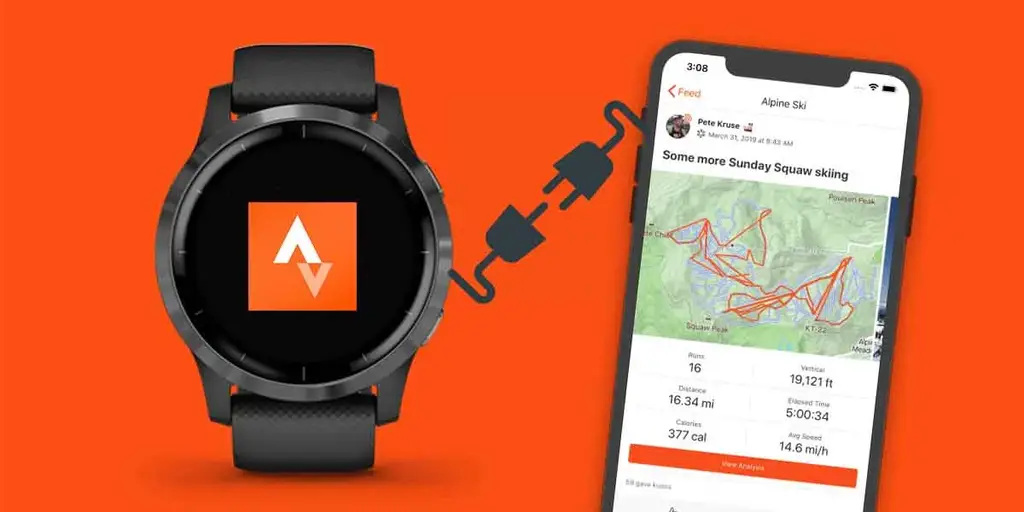
Pulsómetros y relojes deportivos Garmin con Strava - Ofertas para comprar online y opiniones | Runnea

Amazon.com: Coros PACE 2 - Reloj deportivo GPS de alta calidad con correa de nailon o silicona, monitor de frecuencia cardíaca, batería GPS completa de 30 horas, barómetro, conexiones ANT+ y BLE,