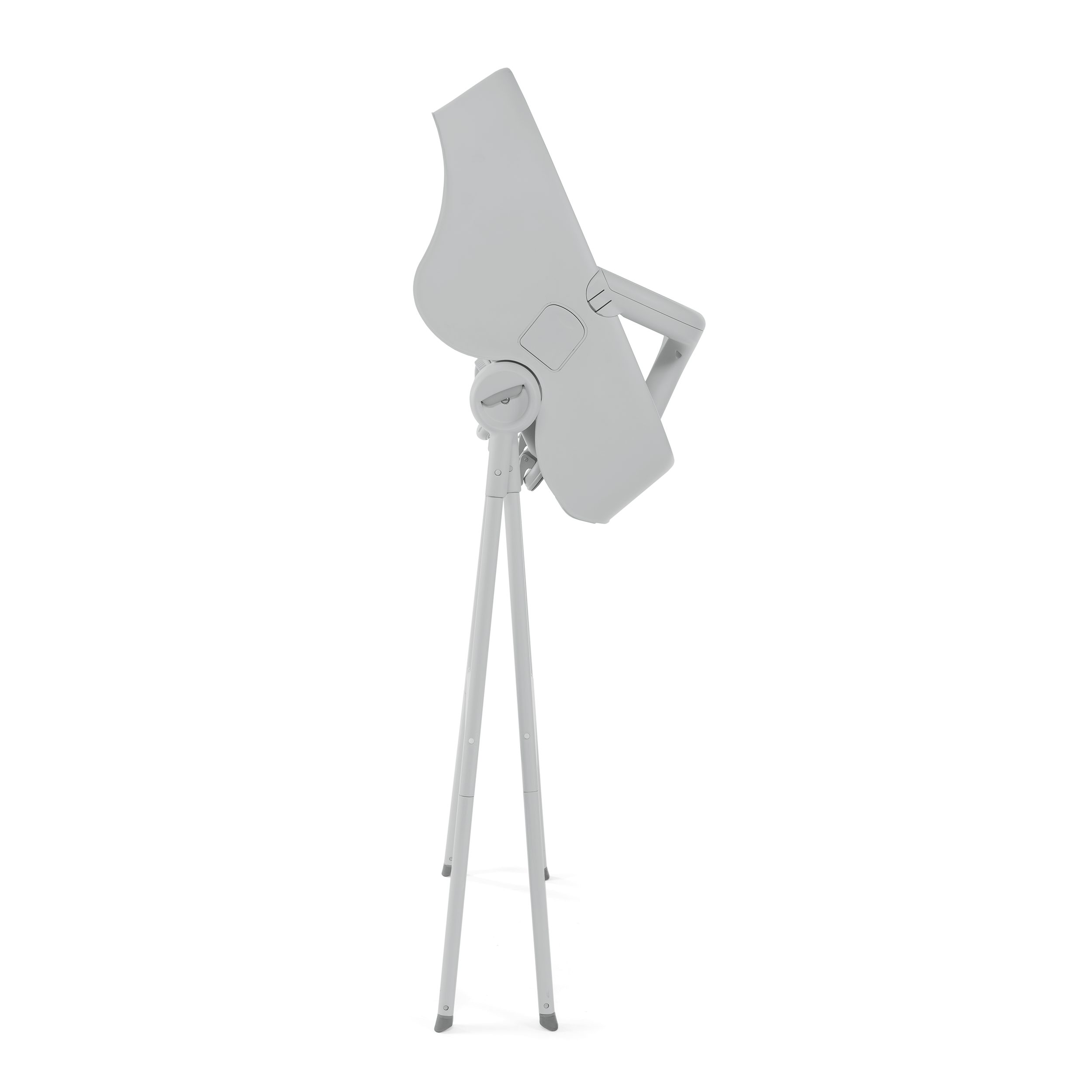
AhLing Wonderland - Bubble Nest est la solution innovante de Chicco qui rendra le moment du bain plus confortable pour les parents et pour bébé ! 💧🚿💧🛁💧 En Vente dans nos 4

Chicco Bubble Nest, Siège de Bain et de Douche pour Bébé, 2 Configurations, Fermeture Compacte, Maximum 11 Kg - de la naissance à 12 mois - Gris : Amazon.fr: Bébé et Puériculture